hidden Accordion
What is Coronary Angioplasty / Stenting?

Coronary Angioplasty (Percutaneous Coronary Intervention) is a minimally invasive procedure that involves inserting a small balloon catheter into a narrowed or blocked artery to improve blood flow to the heart muscles.

A small wire mesh tube, known as a stent, is often implanted during an angioplasty to keep the artery open and reduce the chances of narrowing again. Most modern stents are coated with medication to prevent narrowing within the stent and to keep the artery open.
If you are comparing angioplasty vs stent, it’s important to note that angioplasty refers to the process of widening the artery, while a stent is the device inserted to keep the artery open after widening. In many cases, both are performed together.
Coronary Angioplasty is performed to improve symptoms such as chest pain (angina) and shortness of breath. In emergencies, such as during a heart attack, angioplasty can immediately open a blocked artery, reduce damage to the heart, and be life-saving.

critical narrowing in artery

implanting a stent during PCI
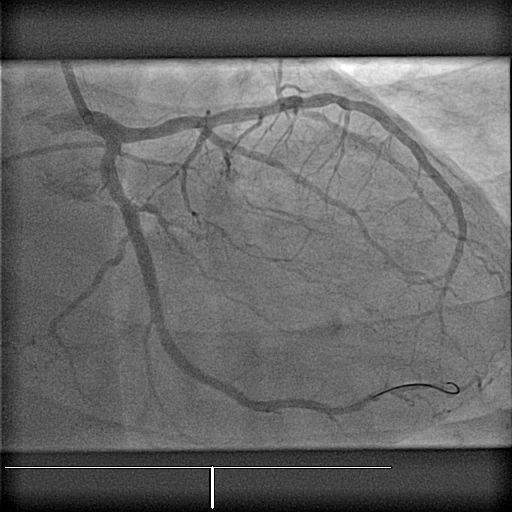
after stenting, normal flow is restored
When is an Angioplasty Needed?
Patients may need angioplasty if:
- They have severely narrowed arteries
- They experience symptoms of coronary artery disease such as chest pain or shortness of breath
- Chest pain is worsening
- They are having a heart attack, where angioplasty can immediately open a blocked artery and limit heart damage
What Causes Narrowed Arteries?
Coronary artery disease occurs when fatty cholesterol deposits (plaque) build up in the arteries, a process known as atherosclerosis. Over time, this narrows or blocks the arteries. Angioplasty treats severe narrowing by opening the affected arteries.

Treatment of Severely Calcified Vessels
Rotational Atherectomy

Source: Boston Scientific Cardiology
Uses a rotating diamond-tipped burr to drill through hardened plaque before stenting.
Orbital Atherectomy

Source: Abbott Vascular
Uses a diamond-coated crown to sand away calcium deposits in the artery wall.
Intravascular Lithotripsy

Uses sonic waves to fracture calcium deposits so stents can be placed effectively.
These procedures may be done before stenting in cases where balloon angioplasty alone cannot open the blockage. Our team will provide guidance on treatment options for these specialised procedures.
Robotic Percutaneous Coronary Intervention (R-PCI)

Dr Joshua Loh also offers R-PCI, allowing precise, remote-controlled manipulation of guidewires and catheters. This combines cardiologist expertise with robotic precision.
Angioplasty vs. Coronary Bypass Surgery
![Coronary Artery Bypass_673828249 [Converted]_Edit-01](https://www.capitalheart.sg/wp-content/uploads/2021/05/Coronary-Artery-Bypass_673828249-Converted_Edit-01-600x375.jpg)
Your cardiologist may recommend bypass surgery instead of angioplasty if there are multiple severe blockages, complex artery structures, or other health conditions. We provide a full breakdown of procedure options, risks, and recovery.
Risks of Angioplasty
Serious complications occur in less than 1% of cases. Other minor issues may include bruising or swelling at the puncture site. Your cardiologist will discuss all aspects of the procedure during your consultation.
Preparing for an Angioplasty
Before scheduling, your cardiologist will review your medical history, perform necessary tests, and discuss the procedure in detail. This includes outlining recovery expectations and giving you clarity on your treatment plan.
Recovery After Angioplasty
You may be discharged the next day if there are no complications. To support recovery, follow heart-healthy habits and attend regular follow-up visits.
References:
https://www.medicalnewstoday.com/articles/327154
https://www.nhs.uk/conditions/coronary-angioplasty/
https://medlineplus.gov/ency/article/007473.htm
https://www.healthline.com/health/heart-attack/angioplasty
https://pubmed.ncbi.nlm.nih.gov/28831994/
https://www.health.harvard.edu/newsletter_article/angioplasty-or-bypass-surgery
https://www.nhs.uk/conditions/coronary-angioplasty/risks/
https://www.mayoclinic.org/tests-procedures/coronary-angioplasty/about/pac-20384761
https://www.nhs.uk/conditions/coronary-angioplasty/recovery
http://secondscount.org/treatments/treatments-detail-2/after-your-angioplasty–stenting-procedure
https://www.healthhub.sg/a-z/diseases-and-conditions/651/coronary-angioplasty-procedure


